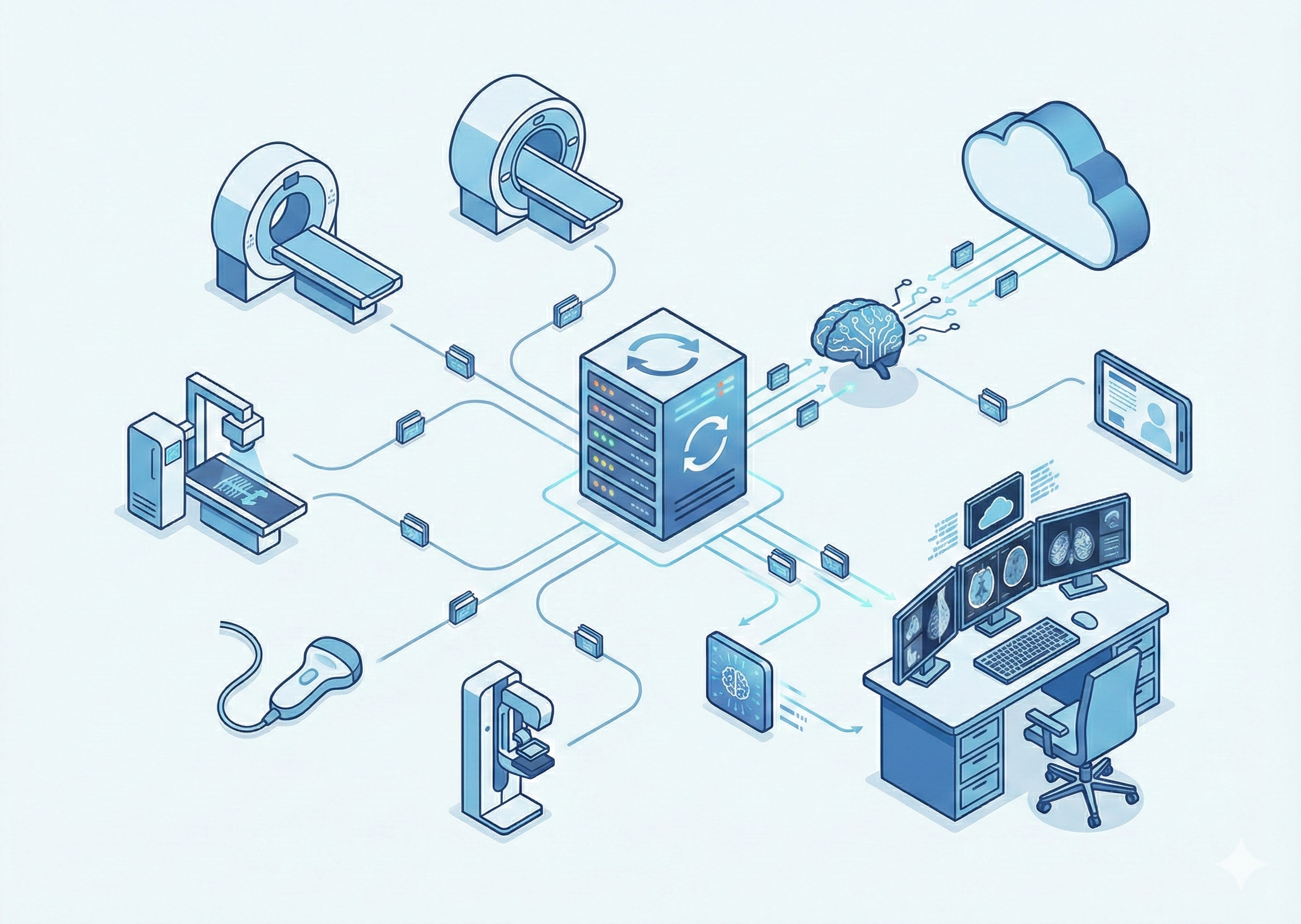
Radiology doesn’t now rely on physical archives and manual data. Today, imaging services employ a high-volume, data-intensive environment. This allows CT, MRI, Ultrasound, X-ray, mammography, and nuclear medicine studies to be accessed real quick, compared over time, interpreted consistently, and retained securely for many years. This shift to a quick approach has turned managing image into a core clinical capability.
At the heart of modern imaging operations Picture Archiving and Communication System (PACS) functions. So, what is PACS? Think of it as a fancy digital storage for medical images. A functioning PACS environment influences how radiologists visualize anatomy, how clinicians collaborate across departments, how studies pass through reporting workflows, if the privacy and security concerns are met, etc. It can also affect how imaging data can support emerging capabilities like AI driven triage and quantification.
This guide takes a hybrid approach. Meaning that, it is clinically grounded and operationally strategic enough (how PACS fits into an enterprise imaging ecosystem). We want you to understand not only what PACS does, but also why it matters and what to consider when modernizing imaging infrastructure.
PACS is a digital system that helps to store, collect, distribute, and view medical imaging studies, using the DICOM standard. But it is more than just some random image storage. PACS in this era improves diagnostic confidence through advanced visualization tools, consistent longitudinal comparison, and collaboration features. PACs support efficient workflows, secure access controls, and integration with RIS/EHR systems as well.
A PACS platform is a system that stores and organizes imaging studies. It offers tools and viewers for interpretation. Most PACS setups connect to imaging devices. They include an image archive that can be on premises, in the cloud, or both. They provide viewers and authorized users with access to studies as needed. PACS platforms are very important for imaging.
PACS uses DICOM for image formatting, metadata, and communication. DICOM is important because it standardizes how images and key details, such as IDs and study descriptions, are packaged and shared. Without DICOM systems, vendors would not work well together. Sharing images would be unreliable. PACS and DICOM work together to make sure images are shared correctly.
It is also important to distinguish PACS from systems. PACS is not the same as RIS.
A Radiology Information System (RIS) primarily manages the workflow. This includes orders, scheduling, worklists, reporting status, and billing-related data. PACS manages the imaging objects and diagnostic viewing. PACS focuses on imaging, while RIS focuses on workflow.
PACS is also not the same as VNA. A Vendor Neutral Archive is usually an enterprise image repository. It stores images from departments, such as radiology, cardiology, endoscopy, dermatology, and pathology. This enables long-term storage and cross-departmental access. PACS is mainly focused on radiology. A VNA can work alongside PACS if a health system wants to manage images beyond radiology.
The Electronic Health Record (EHR) is the system for tracking patient care over time. Integrating PACS with the Electronic Health Record lets clinicians access imaging studies and reports alongside orders, notes, labs, and medications. This means they do not have to switch between systems. PACS and Electronic Health Records work together to make sure clinicians have all the information they need.
The imaging data lifecycle is the process every imaging study follows. This process includes acquisition, transmission, storage, retrieval, review, analysis, reporting, and retention.
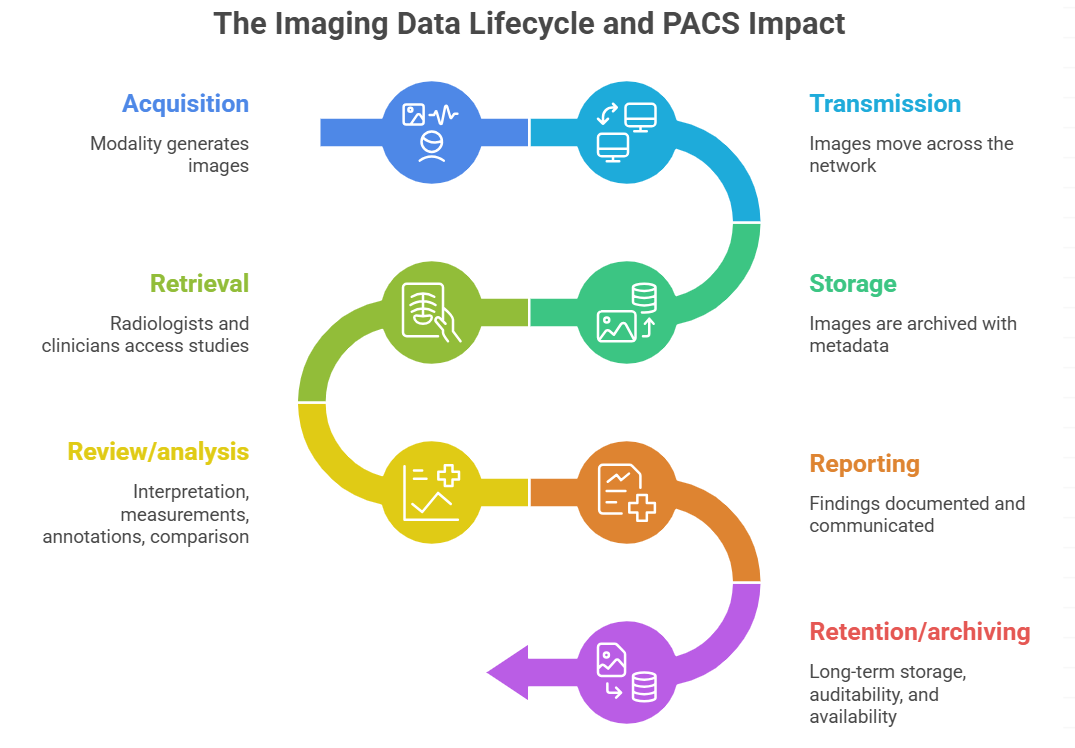
PACS affects every stage of the imaging process. In a department, good performance is essential. Slow systems delay image retrieval. Poor prefetching means previous studies might not be ready when needed. Inefficient image handling can make viewing difficult. If many users access studies at once and the system cannot keep up, everyone slows down. PACS platforms must be able to handle a large volume of images.
High-performing PACS environments often use practical optimizations. These include caching of accessed studies, prefetching of prior exams when a new order arrives, and tiered storage strategies that balance cost and retrieval speed. These optimizations affect how quickly radiologists can move from one study to another. They also influence how reliably clinicians can access images at the point of care. PACS platforms must be optimized for performance.
PACS improves confidence in many clinical situations. Here are some examples.
In trauma and internal bleeding, speed is critical. Trauma CT scans often use multiphase contrast to check for bleeding and blood vessel injuries. PACS tools let radiologists quickly switch between phases, adjust image settings for tissues, and compare series side by side. If a small sign of bleeding appears, fast image review helps the team act quickly. PACS platforms are very important in emergency situations.
In fracture and surgical planning, PACS enables radiologists to review anatomy in different planes. This is important for understanding how bones are displaced, the involvement, and the position of fragments. Measurements and annotations support planning by recording details such as joint step-off, the extent of bone displacement, and alignment. Saving these notes and using the PACS reduces confusion between different readers. It helps keep information clear when patients go to facilities. PACS platforms are very useful for planning.
In chest CT, small changes can matter. A pulmonary nodule may require measurement over time. Interstitial lung disease may require pattern tracking across scans. Pneumonia may require comparison to identify progression or resolution. PACS facilitates comparison by presenting current studies alongside priors. This often uses hanging protocols that keep displays consistent. PACS platforms are very important for tracking changes over time.
Consistency is important for follow-up. When measurement tools are used the same way each time, radiologists can track changes more accurately. Even small gains in consistency can cut down on repeat scans, help doctors understand changes, and lead to follow-up advice. PACS platforms help ensure consistency.
In neuroimaging, reading MRI scans means looking at different image types. PACS viewers help by letting users scroll through images together, use panels, and compare current scans with previous ones. These features are especially useful for stroke, tumor, and demyelinating disease cases. PACS platforms are very useful for neuroimaging.
For example, in suspected acute stroke, rapid identification of diffusion restriction and mismatch patterns can influence treatment windows. In sclerosis, lesion burden and interval change matter, and consistent comparison across time improves clarity. PACS does not diagnose. It makes evidence easier to visualize, compare, and communicate. PACS platforms are very important for diagnosis.
In integration, having ultrasound images integrated in PACS helps teams work together. Obstetric scans may need opinions, vascular studies may need to be compared with other tests, and emergency ultrasounds may need to be documented for later care. PACS keeps all these images secure, just like other types of imaging. PACS platforms are very useful for ultrasound integration.
In oncology follow-up across modalities, PACS helps by making comparisons easier, keeping measurements consistent, and allowing sharing with oncology teams during meetings. This is not about convenience. Having a view over time can improve treatment planning and reduce confusion about what has changed and when. PACS platforms are very important for oncology follow-up.
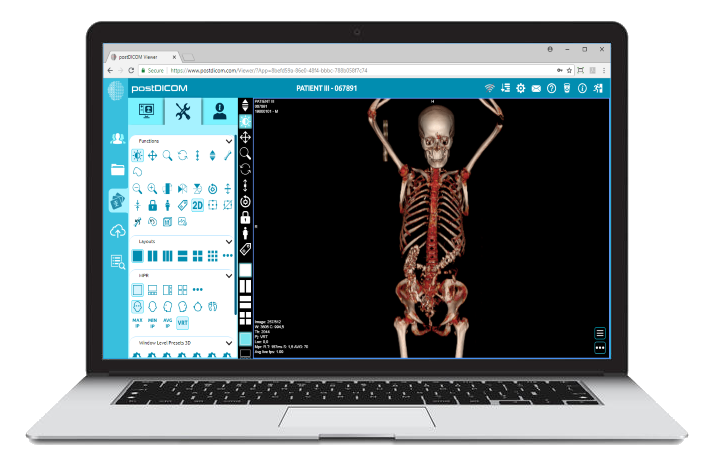
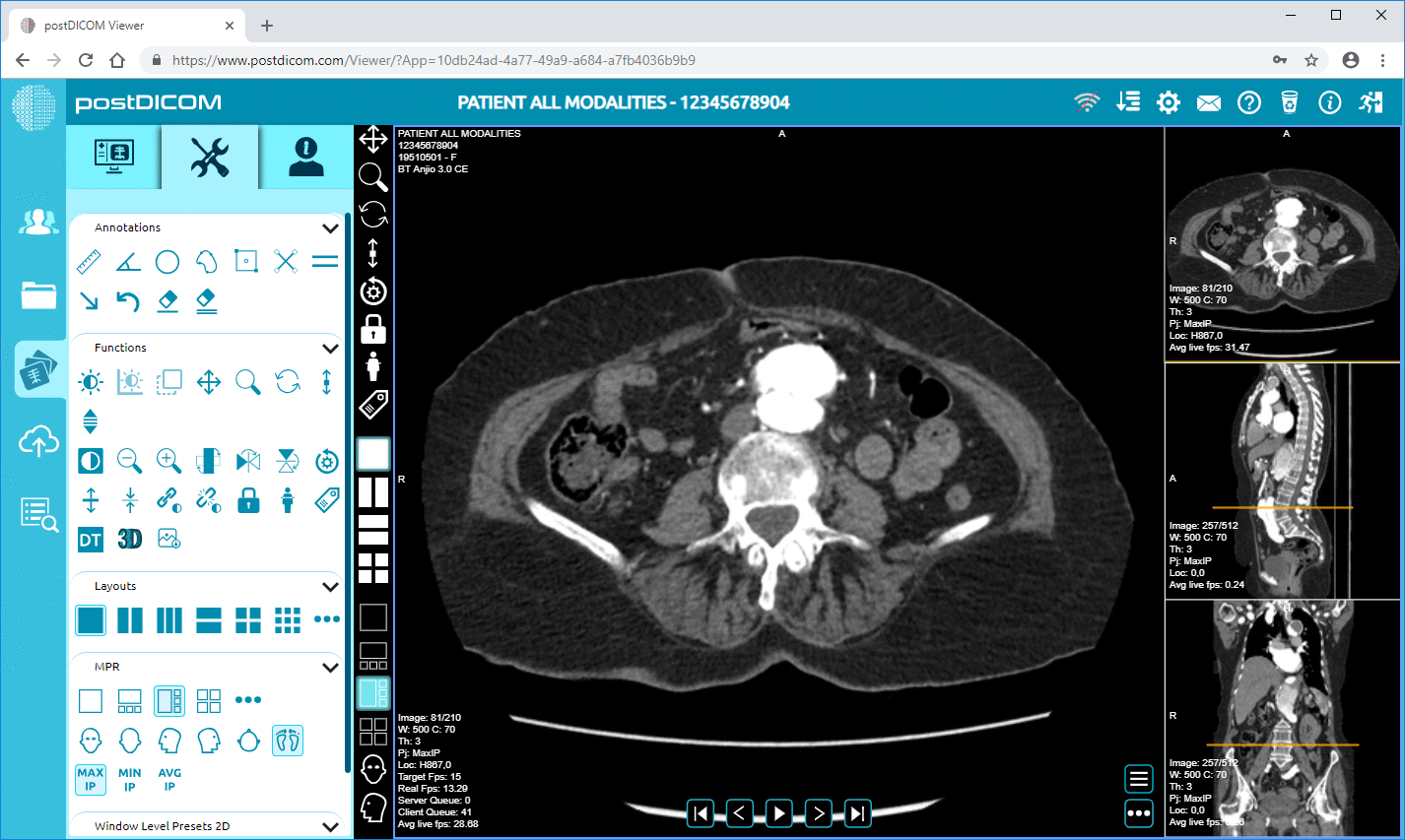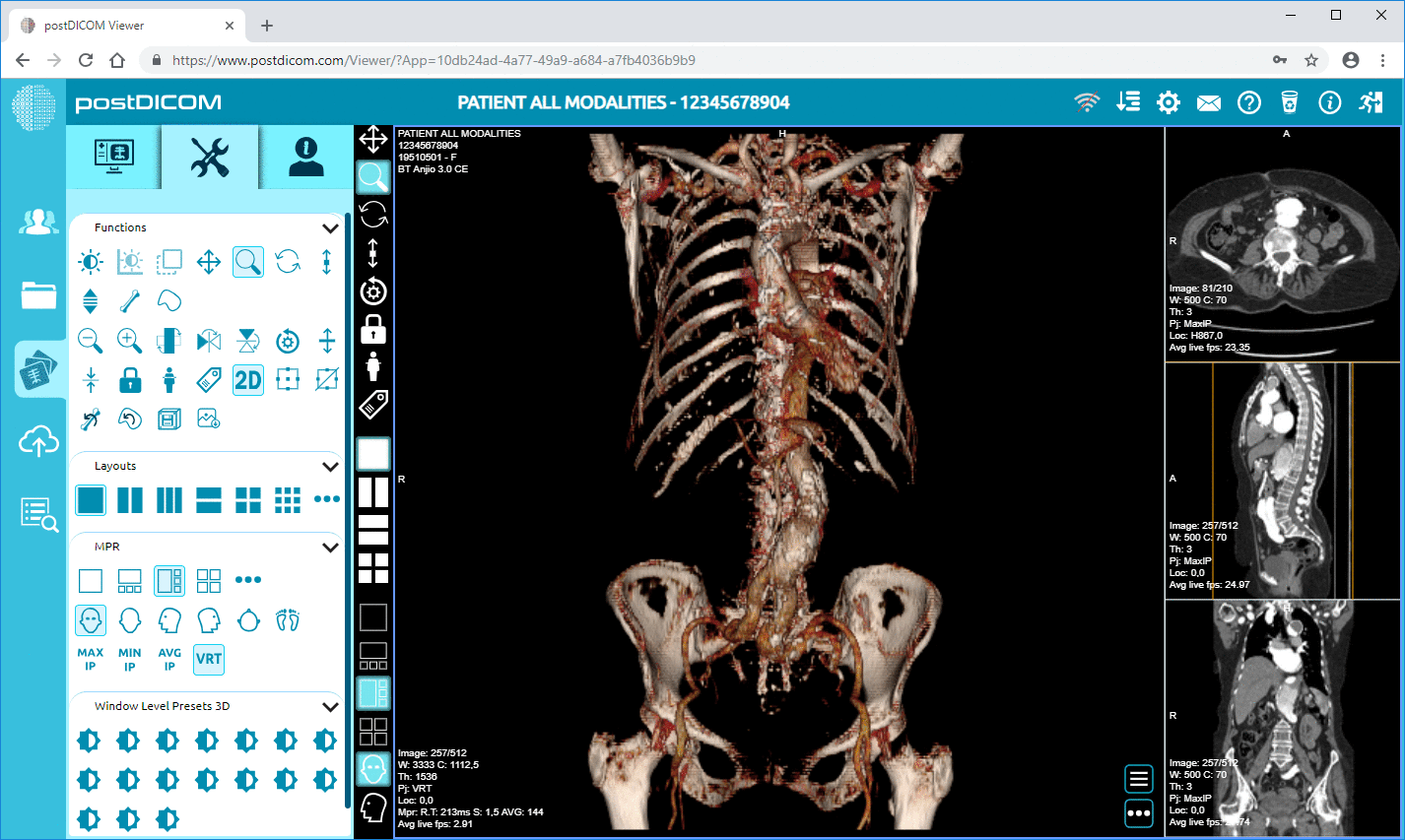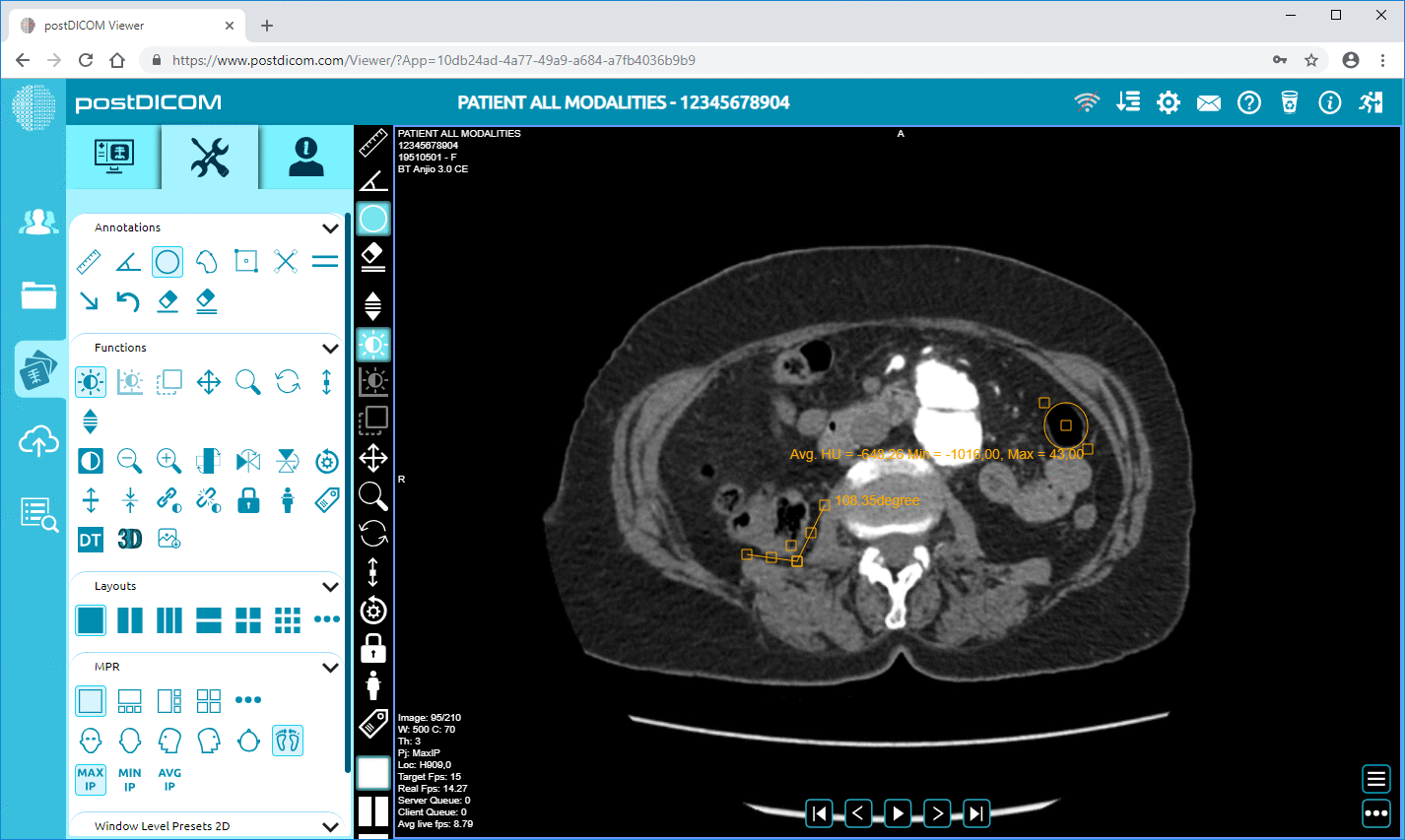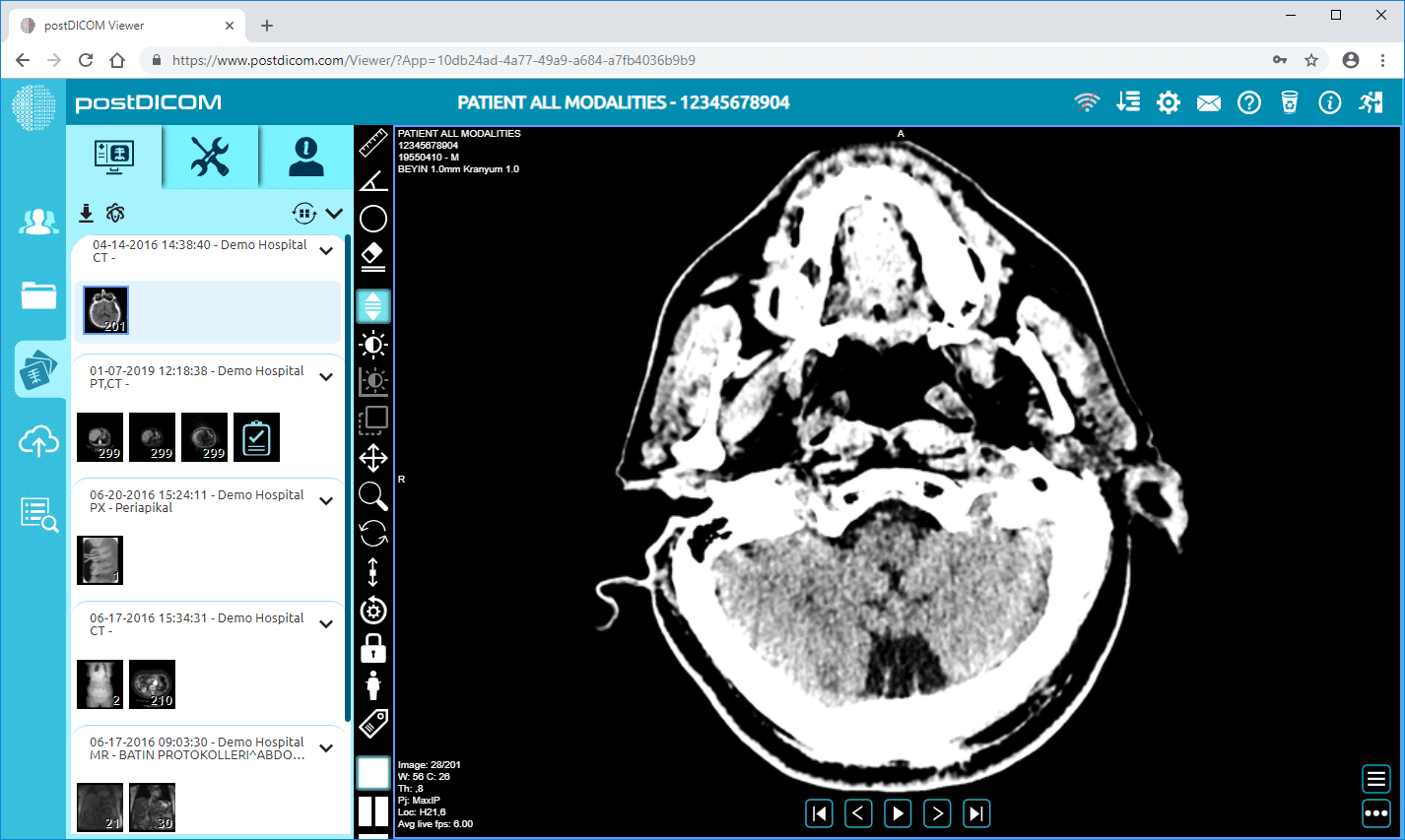
Modern PACS viewers typically include window level presets, high-fidelity magnification, measurements, ROI tools, annotations, key-image workflows, MPR, and 3D rendering. Two features are especially important for authority-grade discussion: hanging protocols and longitudinal comparison workflows.
Hanging protocols standardize how studies open, reducing setup time and improving consistency across readers.
Longitudinal comparison workflows reduce variability. Support more consistent follow-up decisions, especially for chronic disease monitoring. PACS platforms must have these features to be effective.
 - Created by PostDICOM.jpg)
Workflow engineering is the process of designing workflows to reduce bottlenecks. Radiology is a production environment: studies arrive continuously. Throughput matters.
Common bottlenecks include delayed retrieval, manual routing, fragmented access across sites, and interruptions that break reading momentum. PACS addresses these by centralizing access and enabling automation.
Priors can be prefetched so they are ready when the case is opened. Worklists can be routed to subspecialists. Distributed across sites for load balancing. Collaboration tools reduce friction during consultations, and multi-site networks benefit from unified access that reduces duplication and supports standardization. PACS platforms must be designed to reduce bottlenecks.
Interoperability is the ability of systems to work together. Interoperability turns PACS into a tool for the whole organization, not just a single department.
DICOM governs imaging objects so studies can be reliably identified, moved, stored, and retrieved. HL7 supports the exchange of identifiers, encounter details, orders, and reporting status between systems like RIS, PACS, and Electronic Health Records.
When integration is robust, it reduces entry, decreases the risk of mismatched studies, and ensures radiologists see the appropriate clinical context. PACS platforms must be interoperable to be effective.
Security, privacy, and compliance are very important for PACS platforms. Medical images hold health information. And security is not a selling point; it is required by law and for patient care. Good PACS systems use encryption, role-based access, multi-factor authentication, audit logs, and secure remote access controls.
In the EU, organizations must consider principles such as lawful basis, data minimization, access control, and accountability. In the US, HIPAA emphasizes safeguards for protected health information.
Requirements vary by jurisdiction and organization. The operational principle is consistent: protect patient data while enabling appropriate clinical access. PACS platforms must be secure to protect data.
When choosing how to deploy PACS, organizations should use a decision-making process, not just follow trends or slogans.
| Feature | Cloud PACS | On-prem PACS |
|---|---|---|
| Scalability | Elastic storage growth and easier multi-site expansion | Limited by hardware refresh cycles |
| Remote access | Often simpler to support securely at scale | Requires more internal configuration |
| IT maintenance | Vendor-managed infrastructure components (varies by model) | Internal team manages servers/storage |
| Upfront cost | Typically lower capital expenditure | Higher capital expenditure |
| Data residency | Depends on provider regions and contracts | Typically fully internal control |
| Disaster recovery | Often easier to architect replication/failover | Requires local DR build and testing |
Many organizations use a mix of both Cloud PACS and On-prem PACS. The best option for an organization depends on how it works and what rules it must follow.
PACS is very important for the use of Artificial Intelligence in imaging. Artificial Intelligence is increasingly used to enhance images. It helps with looking at images, finding problems, measuring, and deciding what to do. Most Artificial Intelligence tools require images in a format that allows access to the images. PACS helps with this by storing images in one place using formats and controlling who can access the images.
Modernizing PACS often involves migration from legacy systems. That process can be complex: metadata mapping, patient identifier reconciliation, duplicate study handling, and ensuring priors remain discoverable. Imaging teams also must manage change: reading workflows, hanging protocols, training, and adoption.
De-risking commonly includes phased migration, parallel operations, interoperability testing with RIS/EHR, and disaster recovery exercises. Authority content acknowledges these realities because they often determine whether a PACS upgrade succeeds or fails in practice.
| Evaluation area | What to assess | Why it matters |
|---|---|---|
| Performance | Retrieval speed, latency, and concurrency | Drives turnaround and reading efficiency |
| Clinical tools | MPR/3D, measurement, comparison, hanging protocols | Impacts diagnostic confidence and consistency |
| Interoperability | DICOM support, HL7/RIS/EHR integration | Reduces workflow friction and errors |
| Security | Encryption, RBAC, MFA, audit trails | Supports governance and regulatory obligations |
| Scalability | Storage growth, multi-site support | Enables future expansion |
| Disaster recovery | Backups, replication, failover testing | Reduces downtime and data risk |
| Migration plan | Data mapping, priors availability, validation | Protects longitudinal care and continuity |
| Operational fit | Training, support, workflow alignment | Determines adoption success |
PACS is a system. It stores, retrieves. Shows medical imaging studies. PACS uses DICOM standards. It helps radiologists and clinicians share images easily and safely.
PACS helps doctors be more confident in their diagnosis. It allows visualization like adjusting window and level. PACS also helps compare images with new ones. It makes it easier to spot changes and measure things correctly.
RIS handles the tasks. These include scheduling and reporting. PACS handles images. Helps doctors view them. Often PACS and RIS work together. This makes it smooth to order images and get reports.
PACS is mainly for radiology. It helps doctors read images. A VNA stores images from departments. It is not specific to one company. Many hospitals use both. PACS is for radiology. Vna is for long-term storage.
Cloud PACS can be safe. It needs protection like encryption and secure access. Organizations must check rules and contracts. They must make sure they follow regulations.
PACS lets radiologists access images from anywhere. They can use the tools and see old images. This helps with night shifts and specialist reads. It also helps share work between sites.
Many modern PACS work with AI. They share images and control workflows. PACS gives access to data and shows images. Organizations validate AI results.
PACS works with DICOM images. These include X-ray, CT, MRI, ultrasound, and mammography. Support for features may vary.
PACS is not merely a digital archive. It is the infrastructure that enables modern radiology to operate at speed, with consistency, and with secure governance.
Clinically, PACS supports diagnostic confidence through advanced visualization, standardized comparison workflows, and better collaboration. Operationally, it reduces bottlenecks, integrates with RIS/EHR ecosystems, and supports distributed care models such as teleradiology.
Strategically, PACS also serves as a foundation for scalable imaging operations and AI-ready workflows when implemented with careful attention to interoperability, security, and change management.
For organizations modernizing imaging infrastructure, the most durable outcomes come from treating PACS as a clinical-and-operational platform: one that must perform reliably, integrate cleanly, and be governed rigorously.
|
Cloud PACS and Online DICOM ViewerUpload DICOM images and clinical documents to PostDICOM servers. Store, view, collaborate, and share your medical imaging files. |